I-ASC: A Child’s Right to Talk
Since the APPGAT was founded, the group has worked extensively on the issue of augmentative and alternative communication (AAC) technology within the broader sphere of assistive technologies. This continued in 2018, as the APPGAT partnered with Manchester Metropolitan University to disseminate the findings from major new research on symbol communication aids. I-ASC, a three-year NIHR-funded project, explores the decision making process of matching the child to the most suitable communication aid. In collaboration with Manchester Met, the all-party group hosted a daylong conference to explore the findings of the I-ASC research and its resonance with parliamentarians, professionals working in schools, specialist AAC hubs and local NHS services, researchers and funding councils, and including civil servants and civil society organisations, and in particular those who use AAC and their family members, to explore and discuss the research findings.
Opening address
The day began as the APPGAT co-chair Seema Malhotra MP introduced John Bercow MP, the Speaker of the House of Commons, to give the opening address. Seema began by reminding those present that the APPGAT was launched at Speakers’ House and, in the year and a half since then the group has been “growing in its influence and in its reach - and is reaching out and building that vital bridge between Parliament and the sector”. The APPGAT co-chair then addressed The Speakers’ long-standing commitment to the issue of speech, language and communication needs, and remarked that he is “absolutely brilliantly placed to give the opening keynote today to this important conference”.
The Speaker welcomed those present and praised the ‘important 3-year study’. On the topic of identifying appropriate symbol communication aids, he explained that “We have to recognise that there are all sorts of different needs. And policy needs to adjust to needs rather than expecting those people with the needs to adjust to a preordained policy.” The Speaker also highlighted a lack of cohesion between health and education services where there is often “no recognition of the overall need” and “a complete disconnection, particularly at the strategic level, between health education and social care”.
Concluding his remarks The Speaker said “the work that you have done is incredibly important, I'm completely onside with it and always will be” and finally
“I wish you Godspeed. What you are engaged in is a moral mission, and the pursuit of practical improvement. This is about translating an idea, a theory, or a notion, of equality of esteem into practical policy, until we reach a point at which no one ever imagines it would not be this way. We’ve got to get everybody on side, and make everybody aware just what an enormous gap there is between the professionals’ commitment to equality and fairness on the one hand and the all too often evidence of their absence on the other.”
The “ I-A SC explanatory model”
The conference began in earnest with a series of dissemination of talks from the researchers, led by Prof. Janice Murray, Chief Investigator for the I-ASC project (NIHR: Health Services & Delivery Research Project: 14/70/153 - Identifying appropriate symbol communication aids for children who are non-speaking: enhancing clinical decision-making). Prof. Murray began by outlining the collaborative nature of the I-ASC project, which brought together researchers from Manchester Metropolitan University, the University of Leeds, Barnsley Assistive Technology Service, and co-researchers who have lived experience of AAC - either as users of the technology themselves or as parents of people who use AAC.
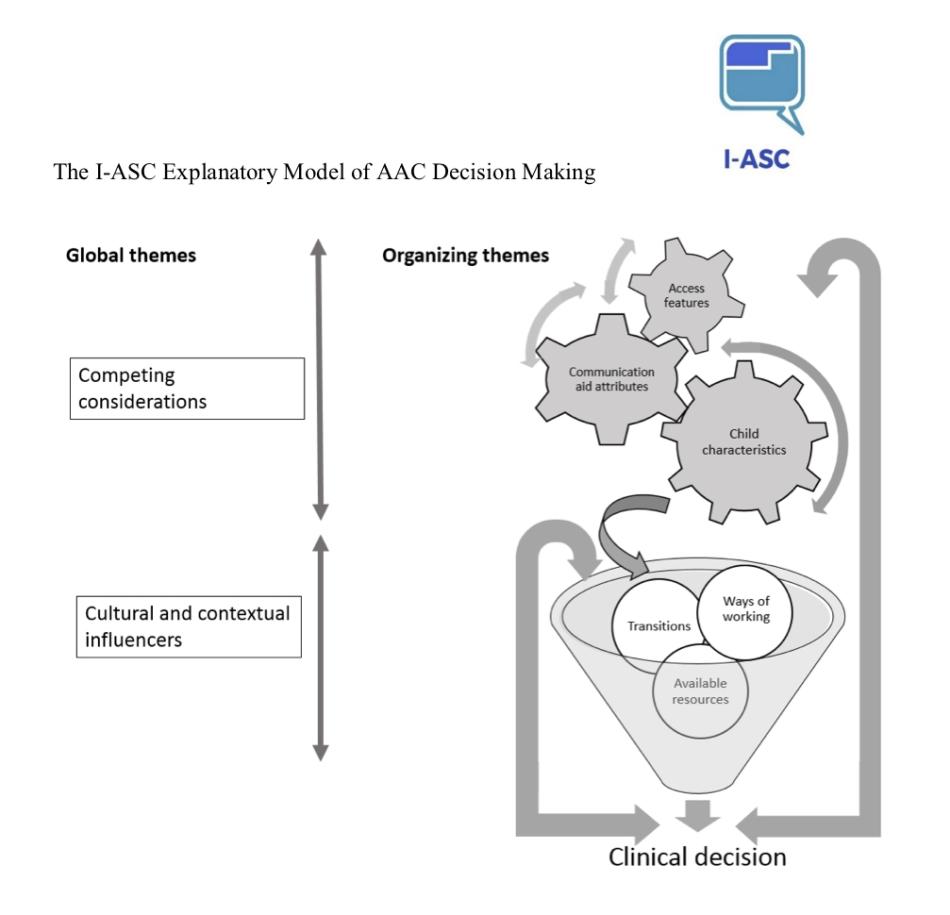
Prof. Murray set out the scale of the project, which is unique both in terms of funding level and of the breadth of data collected: covering the UK as a whole and comprising data sets from focus groups, interviews and quantitative data from surveys. At the heart of the research findings is that AAC recommendation is a “complex area of decision-making: there are a multiplicity of issues, elements that you need to consider and in many instances, you are juggling those”. To capture this, the project developed the “I-ASC explanatory model of clinical decision making”, which as Prof. Murray explained encompasses “competing considerations” and “cultural and contextual influencers”, and the ways each of these factors interact over time.
Dr Yvonne Lynch, a SLT and Research Fellow at MMU, went on to introduce the research findings that relate to how national (UK) policy and guidance for AAC is implemented in practice. As Dr Lynch explained
We would really hope that - based on our national guidance [e.g., in England & Wales, the SEND Code of Practice] - services would be delivered based on child characteristics, driven by the needs of individual children but we are seeing in lots of instances that what’s available in terms of resources is more determined by the way that services have been structured and organised, than who should be involved in communication aid assessments and what that process of recommendation should look like.
Findings from the research show that irrespective of diagnosis “across the dataset, children had very different experiences of communication aid assessment”, including who is involved and how they come to their decisions.
A further finding concerned the cost of communication aids and its influence on decision making. It was clarified that we should distinguish between the extent to which the cost of communication aids may influence commissioning decisions around AAC (i.e., determining the nature of service provision), and the influence of cost at the point of clinical decision making (i.e., within existing UK service provision). Dr Lynch noted that with respect to the second issue, within the I-ASC data, cost “wasn't a big factor for a lot of professionals”: the I-ASC research suggests that once a child has accessed an assessment, clinical decision making does not appear unduly influenced by cost. In this, she pointed out “We are seeing the benefits of those changes that we’ve seen in funding for AAC [which followed the Bercow Review 2018]. If we did this study five years ago it might have been a different picture.”
Dr Edward Webb, a Research fellow at the University of Leeds, explained a methodology that was used by the research team to better understand professionals’ symbol communication aid decision making. I-ASC utilised “discrete choice experiments” to ask participants to choose between a series of different recommendation options for a child vignette. In this case, AAC professionals were given the choice between different sets of communication device features and given some background information about a potential AAC user. Statistical analysis revealed “the interactions between ... preferences for different attributes of AAC systems and characteristics of the child”. Initial findings suggest that professionals pay heed to evidence of existing AAC (lo-tech) progress and relate that to their decisions regarding the introduction of more demanding symbol communication systems.
The final presentation of the morning was from Liz Moulam, a Public Involvement co-researcher at MMU and the parent of a young person who uses AAC. Liz picked up the theme of family involvement in assessment with data that showed family’s views were very diverse. Some saw value in a high degree of involvement while others were happy for professionals to lead the process. The reasons for these family decisions are complex and far ranging, and no/limited involvement in the decision making process is not indicative of no interest in the process and may be more indicative of the complex lives of families who have children with AAC needs.
Liz went on to introduce the methodology of “best-worst scaling” and its use to understand the communication aid preferences and priorities of professionals and families. By analysing how they ranked 18 device characteristics compared to 19 child characteristics. This data was triangulated with opinions collected from parental interviews. The research revealed that “Families often have very different opinions and priorities from professionals”. While all the characteristics identified by the research were recognised as important by both families and professionals, the scaling exercise revealed that “Professionals thought that consistency of layout and navigation, together with vocabulary and language packages, were the most important attributes of the device - and they thought the least important was appearance and voice”, whereas for families “portability, voice, appearance and size were extremely important”.
The I-ASC conclusions from the morning session were considered and debated by an invited panel.
Policy implications
In the final session before lunch, Lord Ramsbotham chaired a panel of experts to discuss the policy implications of these findings. Lord Ramsbotham, who co-chairs the APPG for Speech and Language Difficulties, introduced six panellists, whose engagement on the issues spans health, education and social care:
Anne Longfield OBE (Children’s Commissioner for England)
Prof. Brian Lamb OBE (Chair, Achievement for All)
Kamini Gadhok MBE (CEO, Royal College of Speech and Language Therapists)
Marie Gascoigne (Better Communication CIC)
Sara Bainbridge (Head of Policy and Delivery, NHS Clinical Commissioners)
Prof. Janice Murray (Chief Investigator, I-ASC Project)
Kamini Gadhok began by recalling that, when she practised as a Speech and Language Therapist there was a period when she was involved in supporting children who require AAC. Kamini then addressed the research findings on the context of decision-making around symbol communication aids; she said that some SLTs have reported that
The drive locally is about how many children do you see, not what’s the quality of the intervention or the [therapeutic] outcome. So we [The RCSLT] are also trying to sift [and interpret] some of the data that’s collected through the NHS [so that it’s not] just on numbers but also on outcomes.
She indicated the importance of giving sufficient time to clinical decision making as demonstrated in this research highlighting the complex nature of such decisions. In sum, Kamini addressed the issue of joint-commissioning and identified four “policy levers” that we can use to promote effective commissioning of local services by CCGs. Firstly, the AAC sector can provide guidance and training for CCGs; secondly Ofsted and the Care Quality Commission should make joint commissioning a more explicit consideration in local area SEND inspections; thirdly local joint strategic needs’ assessments should include Speech Language and Communication Needs; and finally, the new CCG Improvement and Assessment Framework should address joint commissioning of SEND services.
Prof. Brian Lamb, opened his remarks by thanking the I-ASC researchers for a "fantastic presentation, and so good to see the way in which you’ve integrated parental and children and young people’s views into the way that the research has been done, which exemplifies… the way that professionals and professional practice should be going."
The I-ASC findings on engaging families in AAC clinical decision making reflected those of the Lamb Inquiry (2009) into Special Educational Needs and Parental Confidence. Prof. Lamb stressed that involving families leads to better more “effective and financially efficient services” and so ultimately better outcomes for children and young people. But to carry out this good practice, we need evidence-based tools for professionals and parents: Prof. Lamb praised the research, “what you're coming up with in terms of a heuristic tool for making decisions, where you can all work together” and explained that this can help services “move from that prescription model of professionals’ work with parents to one that [is] co-production. We’re working on this together to produce a better outcome for that child”. Concluding his remarks, Prof. Lamb extolled the attendees to “use the legislation, use the insights from this brilliant research, use your own great professional practice to go out there [ and make] equality of esteem a reality”.
The Children’s Commissioner for England, Anne Longfield, explained the role she has in promoting good SEND services and advocating for children with SEND. As Commissioner, her role enables her to request information about children's services. Anne pointed out that Professionals need to get alongside families and their children to be able to support children in their usage of assistive technology. The Commissioner then commented upon the I-ASC research findings and the different models of clinical decision-making in AAC. She suggested that the findings indicate that we still need to move away from “the old state [of affairs] where you're waiting for someone to decide what you want, they give you something, it might be something that you do want or you don't want, it might be a halfway house, but it’s ‘doing to’ people, rather than giving them the tools they need to be able to get on and flourish in the best way they can.” Finally, Anne remarked on the I-ASC finding that the size of the team involved in assessment for communication aids varies quite considerably, noting that joint-working is especially relevant in the context of larger teams.
Attendees then heard from Marie Gascoigne who works with CCGs and other stakeholders to improve commissioning of Speech, Language and Communication services across England. Picking up on the issue of joint-commissioning, Marie explained that “there are good examples and we have to be better at gathering and publicizing those” since in many cases, commissioners still don’t know ”what it is they're trying to achieve, so we have to tell them, we have to be very clear in saying this is what a good outcome for children and families looks like”. She suggested that the I-ASC research can make an important contribution to this with its findings on good practice and outcomes in clinical decision making for AAC. Marie continued by indicating that CCG’s need to “set outcome measures that are truly about outcomes and not about counting inputs”. She concluded by indicating that until outcomes are defined, CCGs are unable to effectively design jointly commissioned services with local authorities.
Sara Bainbridge spoke for the association of NHS Clinical Commissioners. Sara began by noting that NHS CCs have two-thirds of the NHS England budget in their control; this shows how important the CCGs are in shaping services such as AAC-related NHS services. “Our members really welcome this research”, Sara said, as Commissioners cannot be experts in all the medical fields in which they commission:
"They obviously have GP's on their leadership bodies but they don't know all the ins and outs as you do, they don’t [necessarily] know what a good [AAC] service looks like. Our members are always crying out for sharing best practice and asking ‘how you can commission a really good service?’."
Sara also assured those in attendance that integration of services is “very much the topic of today” at NHS CC. She suggested that to make this a reality for AAC services, CCGs and Local Authorities need to have the same success measures. In essence, suggesting that it is important to “make sure that each element of the system is held to account and measured. … if you’ve got a CCG that’s being told ‘you’ve got this as your measure of success’ but a local authority has a completely different measure’ [they won’t be able to work together so effectively] having that joined up accountability and measurement will actually really help integration going forward”.
Here again, the I-ASC research was noted as valuable in analysing outcome issues such as technology ‘abandonment’, where the research showed we lack a common definition. Sara confirmed that “having examples [of good practice] like AAC as a joined up [approach, that says] ‘this is what will make a difference for people who have communication needs,” would be helpful for commissioners. Furthermore, “being more person-centred and outcomes focused, is the whole point of integration, so the more research that our members can see like this [i.e., the I-ASC project], the more they’ll be able to put into practice”.
Prof. Murray then joined the panel as the speakers took questions from delegates. The panel and attendees further discussed how to promote joint-commissioning of services - which would help determine the context in which AAC clinical decisions are made. One suggestion was to improve the dissemination of good practice case studies, and, as Sara Bainbridge pointed out, such studies should include reference to commissioning strategy as well as clinical practice and research evidence. Conversely, the pattern of overlap between CCGs and local authorities was identified as a barrier to joint working: Marie Gascoigne explained that some local authorities cover multiple CCG areas, making coordination more difficult. This suggests there is work to be done on understanding how services coalesce for the benefit of the patient/client.
A further topic of discussion was how to evidence positive outcomes and value for money. One concern raised was that, as budgets come under increasing pressure, services may be restructured in ways that offer less value for money - e.g., services may pull back from joint working and investing time in engaging families. The point was made from the floor that evidencing positive outcomes is key to advocating for services. Adding to this, Prof. Murray explained that AAC recommendations take place at different points within a journey that families and young people are on, and so the full outcomes of good practice are seen over the course of a lifetime. How this is effectively captured needs to be revisited within and across services.
The discussion also addressed the nature of the teams involved in AAC recommendation processes. Kamini Gadhok drew attention to the issue of workforce development. She expressed the need for both training of teachers, as advocated by the SEND minister Nadhim Zahawi MP, but also access to SLTs and other specialists [to support the need of these children and young people]. Prof. Lamb continued this theme and pointed out that engaging with families is itself a skill that must be developed and one that pays dividends when it is used effectively. Prof. Murray reflected that each child or young person may have different requirements in terms of their assessment needs, so that we may not be able to fix on a single team size or composition, but we can fix on a comprehensive list of potential contributors and provide a rationale for their involvement.
***
Implications for clinical practice
Following a lunch reception, in which we were joined by members of both Houses, attendees were welcomed back and called to order by Stuart Meredith, an I-ASC co-researcher at MMU and who uses AAC. Stuart explained: “I have been involved in the project even at the design and bidding stage to make sure that all aspects of the project consult people who use AAC”. Once the project was underway, Stuart conducted interviews with families and his speech to the delegates reflected on a variety of different research meetings and interactions with the interviewees, e.g., some interviewees were surprised to find that he was actually conducting the interviews.
Nicola Randall, who is a SLT and Research Associate at the Barnsley Assistive Technology Service, presented some specific applications to clinical practice that built upon the content from the morning sessions. Nicola presented some of the tools that the I-ASC team used to engage children in their research, and she offered suggestions for using the same tools in clinical recommendation assessments to “make sure we hear the perspectives of children and young people who [might] use AAC”. These included communication devices, storybooks about AAC assessments (to introduce the topic and key vocabulary to children) and the “Talking Mats™ approach” (which can be used with children who don’t have a communication device). As Nicola acknowledged, such preparations for data collection require a considerable investment of time. This has implications for clinical practice, as we heard during the earlier part of the day this can be in short supply within services. Yet, the I-ASC findings suggest that “recommendations that reflect the child’s preferences ... are hopefully more meaningful and lasting for them”.
Simon Judge, Head of BATS and a Clinical Scientist, took the podium to comment on some research findings related to attributes of communication aids. In particular, Simon noted that the I-ASC project identified a number attributes that are relevant to the decision making process but also found that the sector lacks common terminology for many features, and that this may hamper attempts to share good practice and assessment tools among professionals. For example, “we know that there has been a proliferation of vocabulary packages and systems that have come into our field recently, and we need a shared language to discuss and evaluate these”.
In a follow up to this anomaly in the AAC field, Liz Moulam turned to the topic of consensus and divergence in group decision-making. Liz presented a tool to capture the different preferences and priorities of stakeholders in the assessment: a spidergram where different considerations are scored by each participant in the assessment. As Liz explained, one can layer the diagrams to identify points of consensus and divergence. Attendees then tested out the tool, each assuming the role of a different person in the recommendation process - e.g. a parent a, teacher, a teaching assistant and SLT. This produced some fantastic discussion and insight.
Prof. Murray followed this with a presentation on the different roles people take in assessment recommendations. The literature review revealed that where team members have a similar level of knowledge and experience, defining roles can be relatively straightforward but where these are variable levels of experience in a team, role definition can be harder. Since assessment teams, with parent involvement, are multi-disciplinary and diverse, this could lead to uncertainty about which roles people should take. Prof. Murray then showed how the spidergram resource discussed above could also be used as a tool to address this challenge. Participants can rate their level of identification with roles such as ‘receiver of information’ and ‘contributor of information’ etc. Finally, Prof. Murray pointed out that understanding roles in this way could facilitate the involvement of a wider group of people, e.g., the driver of the school bus as someone who can contribute some information because they have some interactions with the child.
“If we can get [roles] clear then we are looking towards greater team satisfaction and possibly better outcomes for the young people that we are considering”
This was well received and stimulated lots of debate and reflection concerning the need to define roles and better appreciate the full range of different people’s insights.
I-ASC researcher Helen Whittle presented the final elements of the I-ASC project for the day. Helen explored the study's finding that the means by which decisions are made is not always explicit to all those involved in the process. This is important because “making decisions explicit may offer everyone the opportunity to challenge and amend or agree with those choices and decisions”. Here, again, delegates were shown a tool which is sometimes used in practice: a mind map that records the views of those who took part in the decision. The record can be referred back to in later assessment recommendations or to help inform any ongoing support.
These practice-focused dissemination talks and exercises provided discussion points for our final panel of the day:
Liz Hewson (parent of an adult AAC user)
Carolyn Young (AAC lead Commissioner: NHS England)
Kim Bates (Specialist SLT, Great Ormond Street Hospital)
Dr Michael Clarke (Senior Lecturer, University College London)
Professor Janice Murray (Chief Investigator, I-ASC, Manchester Metropolitan University)
Simon Judge chaired the panel which began with remarks from Carolyn Young, the Lead Commissioner for NHS England Rehabilitation and Disability Specialised services, including AAC. Carolyn thanked the I-ASC team for carrying out this project, adding
I know from my experience when I was asked to take over the commissioning of the specialised services in 2013 that there was a real dearth of research and information from the UK in this area. In the NHS, you won’t be able to deliver any sort of change without having some sort of research and evidence to back it up so research in the area is extremely important.
Carolyn further stressed the impact that the research findings can make on the way services are organised and commissioned; and committed to making use of this new body of evidence: “that is the task I will set myself, along with the specialised AAC group that looks at the services”.
Dr Mike Clark spoke to the relevance of the research to his work as both an academic in the field and a teacher of future SLTs. “It is really a pleasure to see a dynamic theoretical model in the field of AAC, drawn out of real data: he commented. Moreover, he, like Carolyn, pointed to the impact of this research, which he said ‘has the capacity to make a significant change to the way we work’ as ‘it has a very strong applied element as well as a theoretical element’, concluding that the I-ASC Explanatory Model had important “implications for teaching” professionals of the future.
Liz Hewson, the parent of a young man, Toby, who uses AAC, recounted her personal experiences then and now. Liz set out the journey she and her family had taken to access communication devices and the support to use them. Toby, also a delegate at the conference, has used multiple devices to date and thus been involved in several assessment-recommendation processes, each in quite different, and often changing, contexts. As Liz reflected, earlier in the process she had to write to her constituency MP on more than one occasion. Liz stated, “I just wish this research had been done 20 years ago”. Liz continued, Toby’s current device was recommended by one of the specialist [AAC] hubs, and this process was by far the most preferable, including the way in which her family were involved in decision-making. This powerful presentation demonstrated some of the positive developments over the last 20 years, but also challenged everyone to continue to do better.
The last speaker on the panel was Kim Bates, who is an SLT working in the Neurodisability team at GOSH. Kim commented on the I-ASC Explanatory Model which “shows just how complex decisions in AAC are”. She then picked up on the theme of parental involvement in decision-making but explained that this is just one of many important factors in successful assessment and implementation:
“Even the most enthusiastic and on-board parent, if they don’t have buy-in from others in terms of schools, staff support, [etc.], that parental support just isn't enough. So we need to think about support at the assessment-[recommendation] level and specialist service level but also that ongoing support [for families and local teams] to make sure that these devices get used, to support communication.”
This comment echoes the I-ASC finding that decision-making is influenced by a multiplicity of factors, each of which interacts with one another.
Questions and discussion from the floor covered a range of topics including use of the I-ASC resources, non-NHS referrals to AAC hubs, the hub service specification, and the research sample for the I-ASC interviews.
The conference was concluded by Prof Janice Murray who thanked the delegates and praised the partnership of the APPGAT and the I-ASC project.
Those who attended will receive notice of the publication of the research. If you would like to sign up to this list please email robert.mclaren [at] policyconnect.org.uk












